For any pharmacy dispensing controlled substances, DEA recordkeeping is not optional — it is a federal obligation. Violations can result in enforcement actions, registration suspension, or criminal liability. Yet despite the stakes, recordkeeping errors remain one of the most common findings in DEA pharmacy inspections.
This article outlines the core federal recordkeeping requirements that apply to Schedule II controlled substances under 21 CFR Part 1304, explains what records must be maintained and for how long, and clarifies the separation requirements that apply specifically to Schedule II drugs. State-level requirements may impose additional obligations beyond what is described here.
This article is intended for general informational purposes and does not constitute legal advice. Pharmacy registrants are responsible for independently verifying their obligations under all applicable federal and state law.
Why Schedule II recordkeeping is held to a higher standard
The Controlled Substances Act classifies drugs into five schedules based on their potential for abuse and accepted medical use. Schedule II substances — which include opioids such as oxycodone, hydromorphone, and fentanyl, as well as stimulants such as amphetamine and methylphenidate — carry the highest potential for abuse among drugs that have accepted medical applications.
Because of this risk profile, the DEA imposes stricter recordkeeping standards on Schedule II substances than on Schedules III through V. The distinction is not procedural; it reflects the regulatory expectation that every receipt, dispense, and transfer of a Schedule II drug be accounted for with precision and maintained in a form that can withstand DEA inspection.
The six core recordkeeping requirements
Under 21 CFR Part 1304, pharmacies handling Schedule II controlled substances are required to fulfill the following recordkeeping obligations.
- Separate records. Schedule I and II records must be maintained entirely separately from all other controlled substance and business records.
- Initial inventory. A complete physical inventory must be taken on the date the pharmacy first handles controlled substances, per 21 CFR 1304.11.
- Biennial inventory. A complete inventory of all controlled substances in stock must be conducted at least every two years thereafter.
- Receipt records. Every receipt of a Schedule II substance must be recorded, including DEA Form 222 or its electronic equivalent (CSOS).
- Dispense records. Each dispensing must be logged with the drug, quantity, date, patient identifier, prescriber, and dispensing pharmacist.
- Two-year retention. All records must be retained for a minimum of two years and made available to DEA upon request for inspection.

The separation requirement
One of the most frequently misunderstood requirements involves the physical separation of Schedule II records from all other pharmacy records. Under 21 CFR 1304.04, inventories and records for Schedule I and II substances must be kept entirely separate — not merely identifiable or retrievable within a mixed system, but actually separate.
This means that a pharmacy cannot satisfy the requirement by storing Schedule II dispense logs in a shared binder alongside Schedule III–V records, even if the Schedule II entries are clearly labeled. The records must occupy a distinct physical or digital location.
DEA Form 222s — the paper order forms used to receive Schedule II substances — are subject to an additional layer of this rule: they must be maintained separately from all other records, including other controlled substance records. Under 21 CFR 1305.17(c), executed DEA Form 222s must be retained at the registered location for a minimum of two years and be available for inspection.
What must be captured in a dispense record
For each Schedule II dispense, the pharmacy's record must capture sufficient information to reconstruct the transaction. At minimum, this includes:
- Name and dosage form of the controlled substance
- Quantity dispensed
- Date of dispensing
- Identity of the prescribing practitioner
- Patient identifier (typically a prescription reference number)
- Identity of the dispensing pharmacist
Physical inventory: what the count must include
The biennial inventory required under 21 CFR 1304.11 is not a spot check. It must be a complete, documented count of all controlled substances in the pharmacy's possession at the time of the inventory. For Schedule II substances specifically, the count must be exact, not an estimated count.
The inventory must be conducted either at the opening of business or at the close of business on the inventory date. The date and time of the count must be recorded. The inventory must document the drug name, dosage form, strength, and quantity of each substance on hand, and must include any expired or otherwise unusable stock that has not yet been destroyed or transferred.
Recordkeeping software does not replace the physical inventory count requirement. A running digital log of receipts and dispenses is not a substitute for a physical count. Both are required.
Record accessibility and inspection readiness
DEA regulations require that all controlled substance records be made readily retrievable for inspection. For Schedule II substances, this standard is applied strictly: records must be available for immediate review, not located off-site or in storage requiring advance preparation to access.
If records are maintained electronically, the system must be capable of producing readable, printed output. If any code system is used within the record other than pricing information, a key to that code must be maintained alongside the records to ensure full interpretability during inspection.
Pharmacies authorized to use a central recordkeeping location for some records should note that executed DEA Form 222s and physical inventories must remain at the registered pharmacy location. They may not be held at a central recordkeeping site.
State law: an additional layer
The requirements described in this article reflect federal DEA obligations under the Controlled Substances Act and 21 CFR Parts 1304, 1305, and 1306. Most states impose their own controlled substance recordkeeping requirements that may be more stringent than federal law. Some states require shorter retention periods, additional record types, or specific formats for dispense logs.
Pharmacy registrants are responsible for identifying and complying with all applicable state requirements. Federal compliance does not guarantee state compliance, and vice versa.
How C2 Vault supports Schedule II recordkeeping
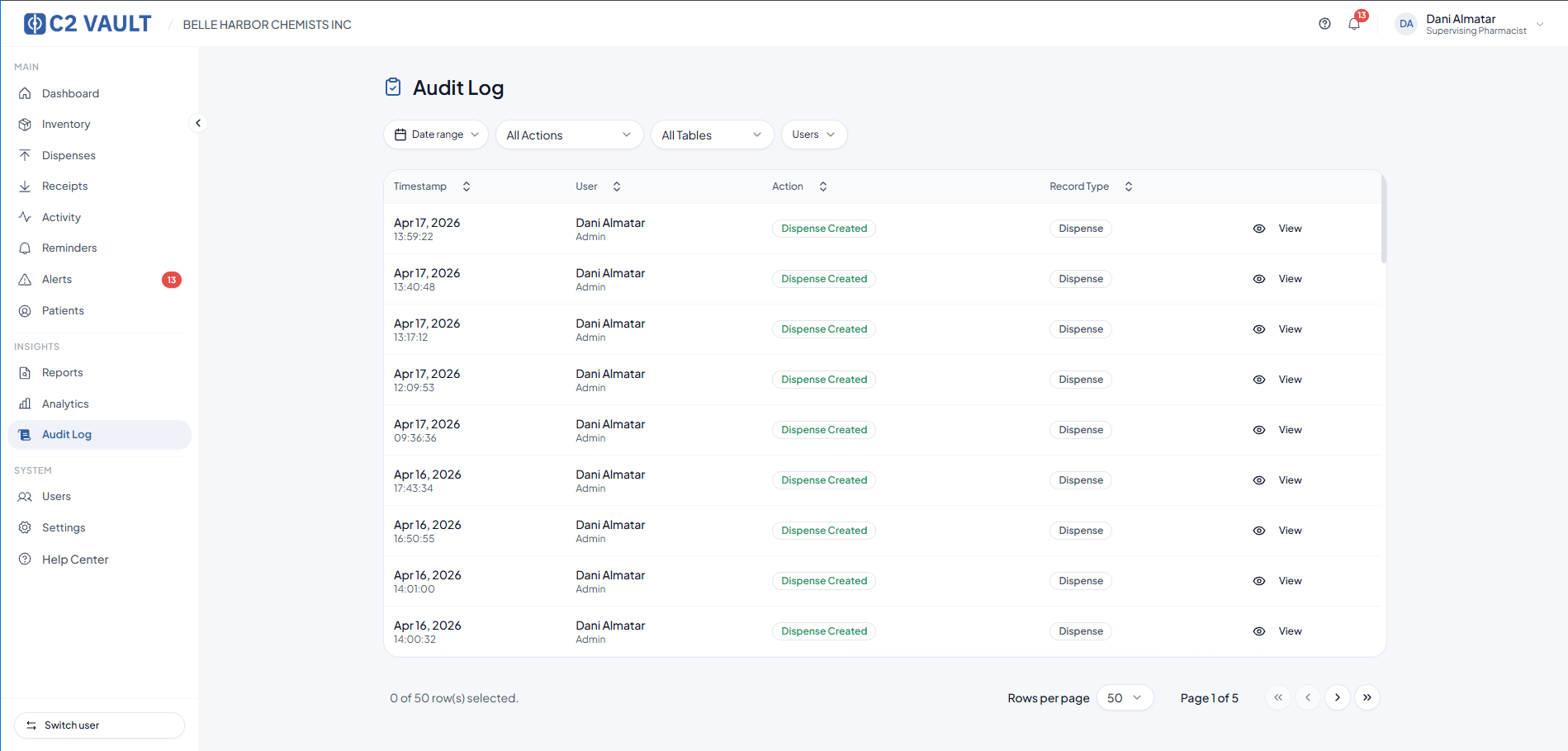
C2 Vault is designed to help pharmacies maintain the structure and accountability that Schedule II recordkeeping demands. The platform logs receipts and dispenses with user-level attribution, maintains a separate, tamper-evident audit trail, and supports the data integrity expected in a DEA-inspectable record system.
C2 Vault does not replace required physical inventory counts, DEA Form submissions, or other regulatory obligations. It is a recordkeeping assistance tool — one designed to reduce the operational burden of maintaining compliant logs while preserving the audit trail integrity that pharmacy registrants are held to.
This article is provided for general informational purposes only and does not constitute legal or regulatory advice. C2 Vault, LLC makes no representations that use of the Application alone ensures DEA or state compliance. Pharmacy registrants remain solely responsible for compliance with all applicable federal and state controlled substance regulations. Consult qualified legal counsel for advice specific to your operations.


